How AI is Revolutionizing Diabetes Diagnosis
Artificial Intelligence is transforming diabetes diagnosis through faster, more accessible, and highly accurate screening tools. From wearable sensors and smartphone-based tests to advanced retinal imaging, AI helps detect early metabolic risks that traditional blood tests often miss—improving early detection and patient outcomes.
Diabetes represents a critical global health challenge. In 2025, 589 million adults worldwide have diabetes, yet over 252 million (≈42%) remain undiagnosed. In the U.S., approximately 37 million adults have diabetes, with 1 in 5 cases going undetected. Traditional screening methods—lab tests like fasting glucose or HbA1c—require clinic visits and often miss early-stage disease. AI-powered diagnostic tools now offer faster, cheaper, and non-invasive alternatives to identify at-risk individuals before symptoms emerge.
Traditional Diagnosis vs AI Insights
Standard diabetes diagnosis relies on blood tests conducted in clinical settings. HbA1c and glucose tolerance tests confirm whether patients meet diagnostic thresholds, but they often fail to capture subtle warning signs of metabolic dysfunction. AI systems, by contrast, can identify hidden patterns that traditional labs overlook.
An AI model using wearable glucose data, diet, and microbiome information could flag early signs of diabetes risk that standard HbA1c tests may miss.
— Scripps Research Scientists
Two patients with identical HbA1c levels may have vastly different underlying metabolic risks. By integrating rich, multidimensional data—such as glucose spike patterns and overnight glucose trends—AI provides clinicians with a more nuanced assessment of metabolic health than any single lab value can offer.
Wearable Glucose Monitors
Automated Machine Learning
Predictive Risk Models

Wearables and Non-Invasive Sensors
AI-enabled wearables and sensor devices are revolutionizing diabetes screening by enabling rapid, accessible testing without needles or clinic visits. These innovations measure biomarkers through breath, light, and video analysis.
Breath Analysis
Acetone detection in exhaled air
Optical Sensing
Smartphone camera PPG signals
Video Diagnostics
Contactless blood flow analysis
Breath Sensor Technology
Researchers at Penn State developed a laser-graphene breathalyzer sensor that detects acetone in exhaled breath—a biomarker of diabetes. When acetone levels exceed ~1.8 ppm, the device flags diabetes or prediabetes. Results are available in minutes with a simple breath sample, eliminating the need for blood draws.
Smartphone-Based Screening
A 2019 Stanford study transformed a popular heart-rate app (Azumio Instant Heart Rate) into a diabetes screener. By shining the phone's flashlight on a fingertip and analyzing the camera's photoplethysmography (PPG) signal, AI detected subtle blood-flow changes caused by elevated glucose levels:
Contactless Video Diagnostics
Japanese researchers developed a contactless approach using high-speed video of the face and hands to capture microscopic blood-flow fluctuations. A deep-learning model analyzed these subtle vascular changes to screen for both high blood pressure and diabetes. The AI "accurately detected the vast majority" of diabetes cases in pilot studies, offering a completely non-contact screening method that could eventually be performed by simply looking into a camera.

Retinal Imaging Meets AI
The retina provides a unique window into systemic vascular health and metabolic dysfunction. AI-powered retinal analysis can now diagnose diabetes—sometimes before patients are aware of their condition—by detecting subtle vascular changes invisible to human examination.
Deep Learning on Fundus Images
A deep-learning model trained on eye fundus photographs achieved an AUC of ~0.86 for distinguishing people with diabetes from those without, even in eyes showing no obvious signs of diabetic retinopathy. The AI identified microscopic vascular alterations that clinicians cannot detect through standard visual inspection.
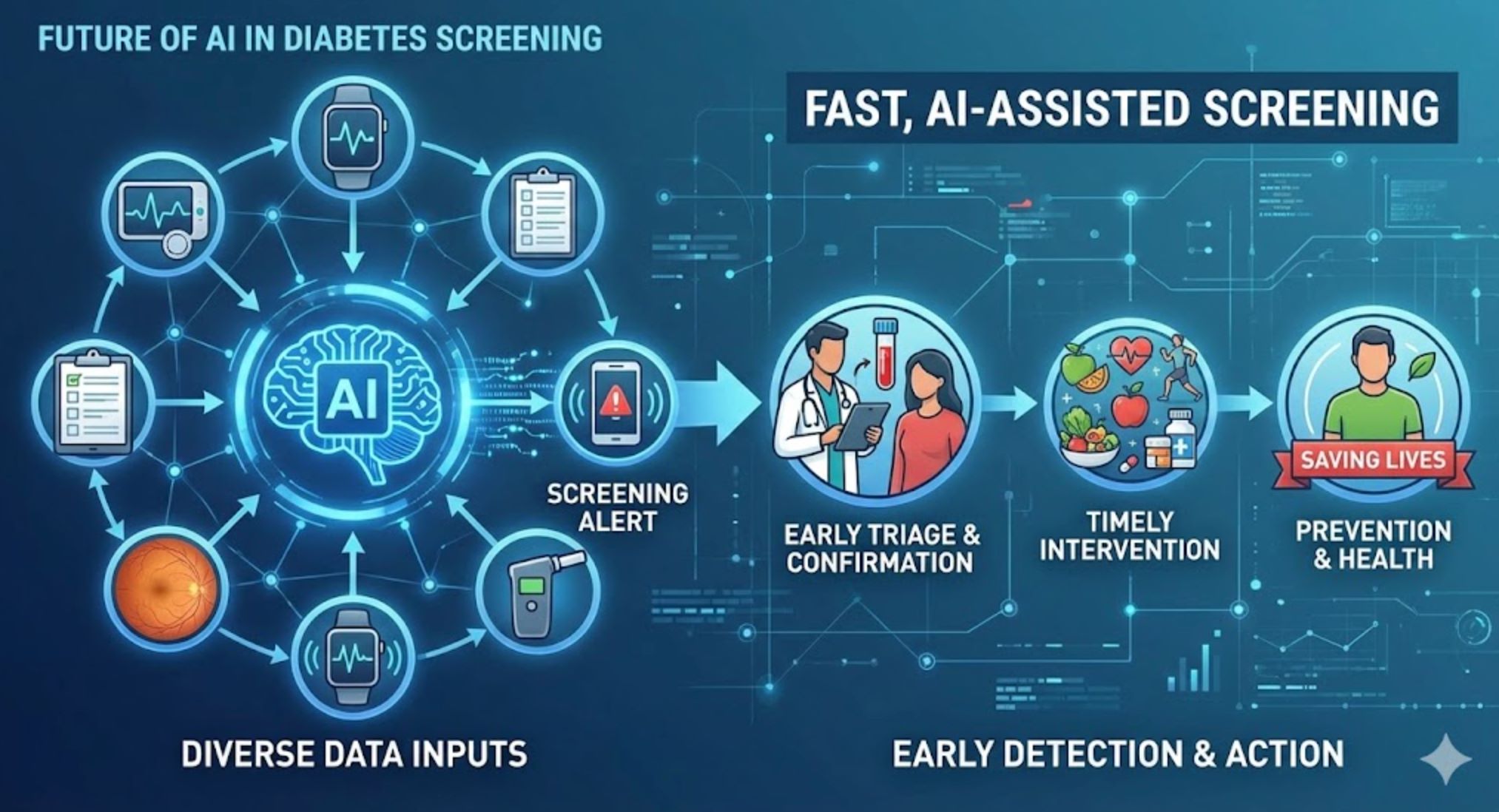
Smartphone Retina Scanning
A novel AI retina app (SMART) processes smartphone camera images in under one second and identifies diabetic eye disease with 99% accuracy. This breakthrough enables:
- Screening by primary-care providers in resource-limited settings
- Self-screening by at-risk individuals at home or in pharmacies
- Global access to diabetes detection for billions of people at minimal cost
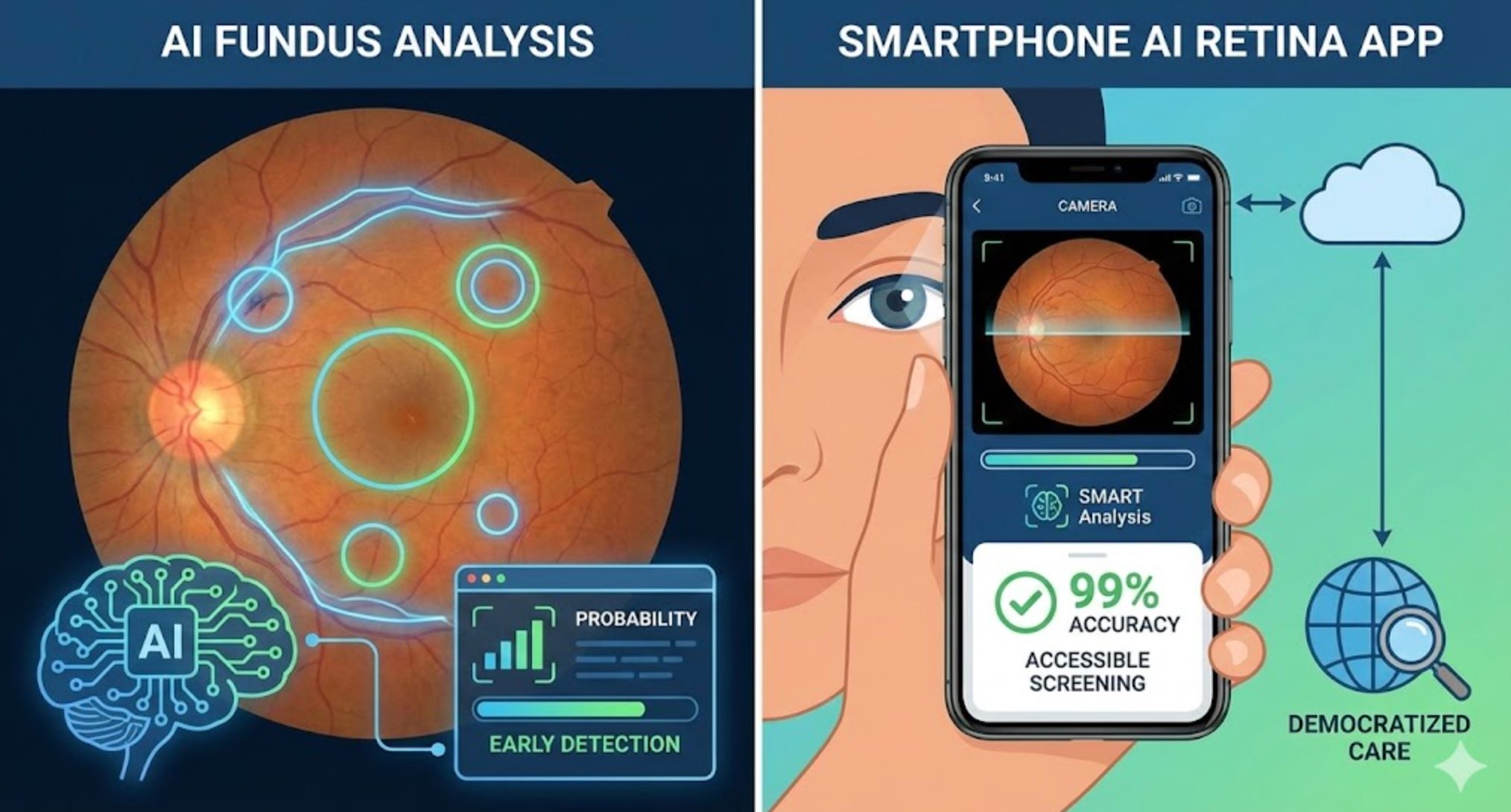
The Future of AI in Diabetes Screening
We are entering a transformative era of fast, AI-assisted diabetes screening. Machine learning models, wearables, and mobile applications can now identify diabetes risk from diverse data sources—continuous glucose patterns, demographic surveys, retinal photographs, breath biomarkers, and more. These tools complement rather than replace clinical judgment, enabling earlier triage and intervention.
Speed
Results in minutes, not days
- Breath sensors: instant results
- Smartphone apps: real-time analysis
- Retinal scans: <1 second processing
Accessibility
Screening anywhere, anytime
- Home-based testing
- Pharmacy screening
- Mobile device compatibility
Cost-Effectiveness
Minimal expense per screening
- No lab infrastructure needed
- Scalable to billions
- Reduced healthcare burden
The Urgency of Early Detection
International health authorities emphasize the critical need for action. The 2025 IDF Diabetes Atlas warns that "over 4 in every 10 people with diabetes [are] not yet diagnosed" and calls for "bolder action" on early detection. AI-driven screening is a cornerstone of this response. By identifying disease earlier, these tools enable timely lifestyle interventions or medications, preventing serious complications and saving lives.
Key Takeaways
- AI detects diabetes patterns that traditional lab tests miss
- Wearables and sensors enable non-invasive, rapid screening
- Smartphone and retinal imaging apps democratize access globally
- Early AI-assisted detection enables timely intervention and prevention
- These tools complement clinical judgment, not replace it
In summary: AI is making diabetes diagnosis quicker, easier, and more widely accessible. From breathalyzers and smartphone apps to advanced retinal analysis, the goal is to find diabetes before it finds you. As these AI tools mature and gain regulatory approval, routine diabetes screening may soon be as simple as blowing into a device or snapping a picture of your eye—bringing hope that fewer cases will ever go undetected.




No comments yet. Be the first to comment!